Hookworm
On this Page
- What is hookworm?
- How is hookworm spread?
- Who is at risk for infection?
- What are the signs and symptoms of hookworm?
- How is hookworm diagnosed?
- How can I prevent infection?
- What is the treatment for hookworm?
- What is preventive treatment?
- What is mass drug administration (MDA)?
What is hookworm?
Hookworm is an intestinal parasite of humans. The larvae and adult worms live in the small intestine can cause intestinal disease. The two main species of hookworm infecting humans are Anclostoma duodenale and Necator americanus.
How is hookworm spread?
Hookworm eggs are passed in the feces of an infected person. If an infected person defecates outside (near bushes, in a garden, or field) or if the feces from an infected person are used as fertilizer, eggs are deposited on soil. They can then mature and hatch, releasing larvae (immature worms). The larvae mature into a form that can penetrate the skin of humans. Hookworm infection is transmitted primarily by walking barefoot on contaminated soil. One kind of hookworm (Anclostoma duodenale)can also be transmitted through the ingestion of larvae.
Who is at risk for infection?
People living in areas with warm and moist climates and where sanitation and hygiene are poor are at risk for hookworm infection if they walk barefoot or in other ways allow their skin to have direct contact with contaminated soil. Soil is contaminated by an infected person defecating outside or when human feces ("night soil") are used as fertilizer. Children who play in contaminated soil may also be at risk.
What are the signs and symptoms of hookworm?
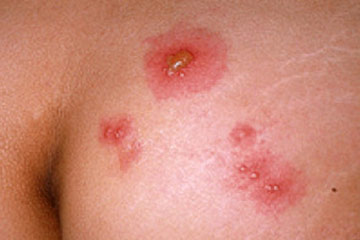
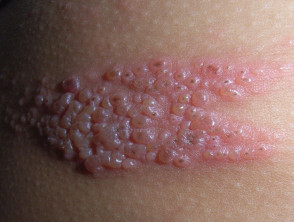
Itching and a localized rash are often the first signs of infection. These symptoms occur when the larvae penetrate the skin. A person with a light infection may have no symptoms. A person with a heavy infection may experience abdominal pain, diarrhea, loss of appetite, weight loss, fatigue and anemia. The physical and cognitive growth of children can be affected.
How is hookworm diagnosed?
Health care providers can diagnose hookworm by taking a stool sample and using a microscope to look for the presence of hookworm eggs.
How can I prevent infection?
Do not walk barefoot in areas where hookworm is common and where there may be fecal contamination of the soil. Avoid other skin-to-soil contact and avoid ingesting such soil. Fecal contamination occurs when people defecate outdoors or use human feces as fertilizer.
The infection of others can be prevented by not defecating outdoors or using human feces as fertilizer, and by effective sewage disposal systems.
What is the treatment for hookworm?
Hookworm infections are generally treated for 1-3 days with medication prescribed by your health care provider. The drugs are effective and appear to have few side effects. Iron supplements may be prescribed if you have anemia.
What is preventive treatment?
In developing countries, groups at higher risk for soil-transmitted helminth infections (hookworm,Ascaris, and whipworm) are often treated without a prior stool examination. Treating in this way is called preventive treatment (or "preventive chemotherapy"). The high-risk groups identified by the World Health Organization are preschool and school-age children, women of childbearing age (including pregnant women in the 2nd and 3rd trimesters and lactating women) and adults in occupations where there is a high risk of heavy infections. School-age children are often treated through school-health programs and preschool children and pregnant women at visits to health clinics.
What is mass drug administration (MDA)?
The soil-transmitted helminths (hookworm, Ascaris, and whipworm) and four other "neglected tropical diseases" (river blindness, lymphatic filariasis, schistosomiasis and trachoma) are sometimes treated through mass drug administrations. Since the drugs used are safe and inexpensive or donated, entire risk groups are offered preventive treatment. Mass drug administrations are conducted periodically (often annually), commonly with drug distributors who go door-to-door. Multiple neglected tropical diseases are often treated simultaneously using MDAs.