Human Papillomavirus (HPV) Vaccine
What is HPV?
HPV (human papillomavirus) is a sexually transmitted virus. It is passed on through genital contact (such as vaginal and anal sex). It is also passed on by skin-to-skin contact. At least 50% of people who have had sex will have HPV at some time in their lives.
Why haven't I heard of HPV?
HPV is not a new virus. But many people don't know about it. Most people don't have any signs. HPV may go away on its own-- without causing any health problems.
Who gets genital HPV?<
Who can get HPV?
Anyone who has ever had genital contact with another person may have HPV. Both men and women may get it -- and pass it on-- without knowing it. Since there might not be any signs, a person may have HPV even if years have passed since he or she had sex.
What makes a person more likely to get HPV?
Most people who have sex may get HPV. You are more likely to get HPV if you have:
- sex at an early age,
- many sex partners, or
- a sex partner who has had many partners.
If there are no signs, why do I need to worry about HPV?
There are many kinds of HPV and not all of them cause health problems. Some kinds of HPV may cause problems like genital warts or cervical cancer. HPV types 16 and 18 cause about 70% of cervical cancers. HPV types 6 and 11 cause about 90% of genital warts.
Is there a cure for HPV?
There is no cure for the virus (HPV) itself. There are treatments for the health problems that HPV can cause, such as genital warts, cervical changes, and cervical cancer.
What should I know about genital warts?
There are many treatment choices for genital warts. But even after the warts are treated, the virus might still be there and may be passed on to others. If genital warts are not treated they may go away, stay the same, or increase in size or number, but they will not turn into cancer.
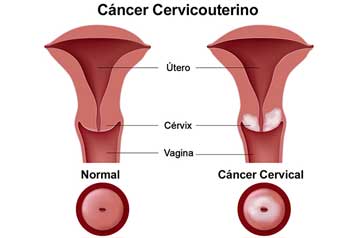
What should I know about cervical cancer?
All women should get regular Pap tests. The Pap test looks for cell changes caused by HPV. The test finds cell changes early -- so the cervix can be treated before the cells turn into cancer. This test also can also find cancer in its early stages so it can be treated before it becomes too serious. It is rare to die from cervical cancer if the disease is caught early.
Is there a test for HPV?
Yes. It tests for the kinds of HPV that may lead to cervical cancer. The FDA approved the HPV test to be used for women over 30 years old. It may find HPV even before there are changes to the cervix. Women who have the HPV test still need to get the Pap test.
Can I lower my chances of getting HPV?
- You can choose not to have sex (abstinence).
- If you have sex, you can limit the number of partners you have.
- Choose a partner who has had no or few sex partners. The fewer partners your partner has had -- the less likely he or she is to have HPV.
- It is not known how much condoms protect against HPV. Areas not covered by a condom can be exposed to the virus.
What is the HPV vaccine and how does it work?
The vaccine mimics the disease and creates resistance. It is NOT a live or a dead virus. It prevents infection with HPV types 6, 11, 16 and 18.
Is it safe?
Tests of the vaccine showed only minor problems. Some people had a slight fever. Others had redness or irritation on their skin where they got the shot.
Is it effective?
The vaccine is between 95-100% effective against HPV types 6, 11, 16, 18.
Who should get the HPV vaccine?
The FDA has approved the vaccine for girls and women ages 9-26. It is best to get the shot before the start of sexual activity.
How many shots do you need?
There are three shots. Once you get the first shot, you need a second shot two months later. You need to get a third shot six months after you get the first shot.
How long are you protected?
Since the vaccine is new, more studies need to be done. For example, the FDA does not know if you will need to have a booster after a couple of years.
Should I get the vaccine if I already have HPV?
The vaccine will not treat or cure HPV. It may help people who have one type of HPV from being infected with the other types. For example, if you have type 6, it may protect you from getting type 16.
Can I catch HPV from getting the vaccine?
No. The vaccine does not contain the HPV virus.
HPV Vaccine Recommendations From the American Academy of Pediatrics (March 1, 2012):
-
Girls 11 through 12 years of age should be immunized routinely with 3 doses of HPV4 or HPV2, administered intramuscularly at 0, 1 to 2, and 6 months. The vaccines can be administered starting at 9 years of age at the discretion of the physician.
-
All girls and women 13 through 26 years of age who have not been immunized previously or have not completed the full vaccine series should complete the series.
-
Boys 11 through 12 years of age should be immunized routinely with 3 doses of HPV4, administered intramuscularly at 0, 1 to 2, and 6 months. The vaccine can be given starting at 9 years of age at the discretion of the physician.
-
All boys and men 13 through 21 years of age who have not been immunized previously or have not completed the full vaccine series should receive HPV4 vaccine.
-
Men 22 through 26 years of age who have not been immunized previously or have not completed the full vaccine series may receive HPV4 vaccine. Cost-efficacy models do not justify a stronger recommendation in this age group.
Anuncios -
Special effort should be given to immunizing men who have sex with men up to 26 years of age who have not been immunized previously or have not completed the full vaccine series.
-
Previous sexual activity is not a contraindication to HPV immunization or completion of the immunization series. Patients infected with 1 HPV type may still benefit from protection against remaining HPV types in the vaccine. Testing for previous exposure to HPV is not recommended. HPV vaccine can be administered when a female patient has an abnormal or equivocal Papanicolaou test result. There is no known therapeutic (as opposed to prophylactic) benefit from the HPV vaccines.
-
HIV-infected people of either gender, 9 through 26 years of age, who have not been immunized previously or have not completed the full vaccine series should receive or complete their series with HPV4.
-
HPV vaccines can be administered at the same visit as all other recommended vaccines.
-
HPV vaccine can be administered in these special circumstances:
-
a. when a patient is immunocompromised because of disease or medication
-
b. when a female patient is breastfeeding
-
- PV vaccine is not recommended during pregnancy. The practitioner should inquire about pregnancy in sexually active female patients, but a pregnancy test is not required before starting the immunization series. If a vaccine recipient becomes pregnant, subsequent doses should be postponed until completion of the pregnancy. It is recommended that women who become pregnant while receiving HPV vaccine be reported to registries that have been developed to record data on outcomes (HPV2: 1-888-452-9622; HPV4: 1-800-986-8999).
-
Because HPV vaccine will not prevent infection attributable to all high-risk HPV types, cervical cancer screening recommendations (ie, Papanicolaou testing) should continue to be conducted in women who have received HPV vaccine.
-
Administration of HPV vaccine does not change current counseling recommendations for use of barrier methods for the prevention of HPV and other sexually transmitted infections as well as discussion about healthy choices about sexual activity, including condoms and abstinence.
-
HPV immunization of children 9 years of age and older should be covered by all public and private health insurers.
CONTRAINDICATIONS
HPV4 should not be given to people with a history of immediate hypersensitivity to yeast or to pregnant women.
PRECAUTIONS
Immunizations should be deferred for people with moderate or severe acute illness. Because syncope can occur in adolescents after injections and has been reported after HPV vaccine, vaccine recipients should sit or lie down for 15 minutes after administration.
Source
- US Food And Drug Administration
http://www.fda.gov/womens/getthefacts/hpv.html - American Academy of Pediatrics. HPV Vaccine Recommendations. http://pediatrics.aappublications.org/content/129/3/602.full
GeoSalud, January 24, 2014
Related Topics
More Topics
-
Human Papillomavirus
-
Human Papillomavirus Vaccines: Questions and Answers
-
Human Papilloma Virus Signs and Symptoms
-
Human Papillomavirus Screening
-
Human Papillomavirus Treatment
-
Human Papillomavirus Prevention
-
Human Papillomavirus and Men
-
HPV and Men
-
Human Papillomavirus Infection Treatment
-
Human Papillomavirus Vaccine
-
Human Papillomavirus and Genital Warts
-
Human Papillomavirus Associated Cancers
United States, 2004–2008 -
Preventing Cervical Cancer Worldwide (PDF document)
-
FDA Advisory Panel Recommends Human Papillomavirus Vaccine